Created by Gary B. Rollman, Emeritus Professor of Psychology, University of Western Ontario (In addition to links below, see weekly archives in the right column)
Tuesday, December 28, 2010
Chronic Pain Policy Coalition - U.K.
Improving chronic pain management through treatment and education | PainEDU.org
Let's Talk Pain Medication Safety Series
PainSAFE Home Page
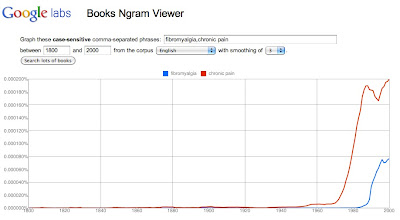
Google Ngram Viewer - pain term trends
Friday, December 24, 2010
Meet the Ethical Placebo: A Story that Heals | NeuroTribes
A provocative new study called "Placebos Without Deception," published on PLoS One today, threatens to make humble sugar pills something they've rarely had a chance to be in the history of medicine: a respectable, ethically sound treatment for disease that has been vetted in controlled trials.
The word placebo is ancient, coming to us from the Latin for "I shall please."As far back as the 14th Century, the term already had connotations of fakery, sleaze, and deception. For well-to-do Catholic families in Geoffrey Chaucer's day, the custom at funerals was to offer a feast to the congregation after the mourners sang the Office for the Dead (which contains the phrase placebo Domino in regione vivorum, "I shall please the Lord in the land of the living"). The unintended effect of this largesse was to inspire distant relatives and former acquaintances of the departed to crawl out of the woodwork, weeping copiously while praising the deceased, then hastening to the buffet. By the time Chaucer wrote his Canterbury Tales, these macabre freeloaders had been christened "placebo singers."
In modern medicine, placebos are associated with another form of deception — a kind that has long been thought essential for conducting randomized clinical trials of new drugs, the statistical rock upon which the global pharmaceutical industry was built. One group of volunteers in an RCT gets the novel medication; another group (the "control" group) gets pills or capsules that look identical to the allegedly active drug, but contain only an inert substance like milk sugar. These faux drugs are called placebos.
Inevitably, the health of some people in both groups improves, while the health of others grows worse. Symptoms of illness fluctuate for all sorts of reasons, including regression to the mean. Since the goal of an RCT, from Big Pharma's perspective, is to demonstrate the effectiveness of a new drug, the return to robust health of a volunteer in the control group is considered a statistical distraction. If too many people in the trial get better after downing sugar pills, the real drug will look worse by comparison — sometimes fatally so for the purpose of earning approval from the Food and Drug Adminstration.
For a complex and somewhat mysterious set of reasons, it is becoming increasingly difficult for experimental drugs to prove their superiority to sugar pills in RCTs, which was the subject of an in-depth article I published inWired called "The Placebo Problem," recipient of this year's Kavli/AAAS Science Journalism of the Year award for a magazine feature.
Only in recent years, however, has it become obvious that the abatement of symptoms in control-group volunteers — the so-called placebo effect — is worthy of study outside the context of drug trials, and is in fact profoundly good news to anyone but investors in Pfizer, Roche, and GlaxoSmithKline. The emerging field of placebo research has revealed that the body's repertoire of resilience contains a powerful self-healing network that can help reduce pain and inflammation, lower the production of stress chemicals like cortisol, and even tame high blood pressure and the tremors of Parkinson's disease.
Jumpstarting this network requires nothing more or less than a belief that one is receiving effective treatment — in the form of a pill, a capsule, talk therapy, injection, IV, or acupuncture needle. The activation of this self-healing network is what we really mean when we talk about the placebo effect. Though inert in themselves, placebos act as passwords between the domain of the mind and the domain of the body, enabling the expectation of healing to be translated into cascades of neurotransmitters and altered patterns of brain activity that engender health.
That's all well and good, but what does it mean in the real world of people getting sick? You can hardly expect the American Medical Association to issue a wink and a nod to doctors, encouraging them to prescribe sugar pills for seriously disabling conditions like chronic depression and Parkinson's disease. Meanwhile, more and more studies each year — by researchers like Fabrizio Benedetti at the University of Turin, author of a superb new book called The Patient's Brain, and neuroscientist Tor Wager at the University of Colorado — demonstrate that the placebo effect might be potentially useful in treating a wide range of ills. Then why aren't doctors supposed to use it?
The medical establishment's ethical problem with placebo treatment boils down to the notion that for fake drugs to be effective, doctors must lie to their patients. It has been widely assumed that if a patient discovers that he or she is taking a placebo, the mind/body password will no longer unlock the network, and the magic pills will cease to do their job.
Thursday, December 23, 2010
Have you ever been in so much physical pain that you actually considered suicide? : AskReddit
Last night after some mild delusions I actually was ok with the idea of shooting myself in the head and just be able to sleep.
edit: Also, im purple-red from throwing up so much. I feel like I fell asleep on the beach with the sun hitting me for 3 days straight
http://www.reddit.com/r/AskReddit/comments/epcnl/have_you_ever_been_in_so_much_physical_pain_that/
Wednesday, December 22, 2010
Chilli compound helps identify pain genes - Science, News - The Independent
The compound which gives chillies their kick is being used in the fight against chronic pain.
Researchers at Aberdeen University have identified how genes are "turned on" to make humans feel pain.
Capsaicin, the compound in chillies which gives them their kick, can also turn on the switch.
It is believed the study could herald the development of new painkilling drugs.
The team looked at the mechanics of the pain gene known as substance-P which was first associated with chronic inflammatory pain more than 30 years ago.
Genes need "switches", known as promoters and enhancers, to turn them on in the right place, at the right time and at the right level.
One of the major findings of the study was that the switches do not act in isolation and need other switches to "speak to" in order to activate the gene.
Researchers based in the university's Kosterlitz Centre for Therapeutics spent five years looking for the switches that turn the substance-P gene on in a group of cells called sensory neurones.
Dr Lynne Shanley said: "Finding the switch was like looking for a needle in a haystack.
"However, by comparing the genetic sequences of humans, mice and chickens, we were able to find a short stretch of DNA that had remained unchanged since before the age of dinosaurs.
"We were delighted when this little bit of DNA turned out to be a genetic switch, or enhancer sequence, which could turn on the substance-P gene in sensory neurones."
Marissa Lear, head technician on the project, said: "Because the switch was active in these sensory neurones we applied capsaicin, the 'hot' chemical in curry and chilli, to see if the switch could be turned on and, amazingly, it was."
Chronic inflammatory pain in the form of arthritis and other conditions affects thousands of people in the UK each year and in many cases is untreatable.
Capsaicin has previously been used as treatment for chronic pain.
The scientists said understanding the genetic mechanisms that allow capsaicin to induce inflammatory pain will lead to a better understanding of the pain process.
Professor Ruth Ross, head of the Kosterlitz centre and a co-author of the paper, said: "Understanding the genetic processes that trigger inflammatory pain is essential to developing new therapies.
"Finding this new substance-P enhancer sequence, and showing that it can respond to capsaicin, has allowed us to add another part of the complex jigsaw puzzle that makes up the inflammatory pain response."
The findings are published in the journal Neurosignals.
http://www.independent.co.uk/news/science/chilli-compound-helps-identify-pain-genes-2166010.html
US Drug Watchdog Urges All Facebook & Social Network Users To Tell Their Friends About The Darvocet & Darvon Pain Pill Recall & Severe Heart Damage
Friday, December 17, 2010
The Alabama pain-relief cartel. - By Timothy Noah - Slate Magazine
In my previous column ("Populists v. Consumers"), I suggested that "regulation" and "consumer protection" meant the same thing. That was a slight oversimplification. Regulation is supposed to mean the same thing as consumer protection, but sometimes it falls short of that ideal. In the absolute worst instances, regulators are so thoroughly captured by the interests they regulate that they create regulations more likely to harm consumers than help them. A good example at the state level surfaced on Nov. 3 when the Federal Trade Commission's Office of Policy Planning sent a letter to Patricia Shaner, general counsel for Alabama's State Board of Medical Examiners.
The FTC was troubled by a regulation that Alabama's state medical board proposed in July stating, "The interventional treatment of pain may be performed and provided only by qualified, licensed medical doctors and doctors of osteopathy" because it "constitutes the practice of medicine." The purpose of the proposed rule is to prevent nurse practitioners from doing something they've been doing in most states for a very long time: managing patients' pain.
The Alabama medical board's justification for proposing the rule is that allowing "unqualified providers" to perform interventional pain management (a category that includes "needle placement to inject drugs" through the skin, epidural injections, and injection of analgesics and anesthetics, among other procedures) "presents serious risk to patients, such as persistent or worsened pain, bleeding, infection, nerve damage, brain damage, paralysis or even death." Sounds scary, right? But as the FTC noted in its letter, Alabama has a category of nurse called a Certified Registered Nurse Anesthetist. CRNAs are trained and state-certified to perform the very tasks that the state now proposes to restrict to medical doctors. Delegating this task to nurses is hardly unusual; as anyone who's been in a hospital lately knows, it is nurses, not doctors, who typically manage pain. Doctors tend to regard pain and its treatment as a bit … pedestrian. It really only interests them as a diagnostic indicator. You want somebody to make the pain stop right away, call the nurse.
My wife died six years ago after a long illness. During one hospitalization she told a doctor making the rounds that she was in pain. The doctor replied with a lengthy monologue about what she might expect to feel after her recent procedure, and ended with the admonition that if she experienced any pain whatsoever she should be sure to tell him. An awkward silence ensued. Finally, the nurse chimed in: "She just did."
There is one category of doctors who are very interested in pain: anesthesiologists. Anesthesiologists typically enjoy predictable work schedules and earn a mean income of $211,750, compared with $63,750 for registered nurses. A study by the Lewin Group found that allowing CRNAs to provide anesthesia was especially cost-effective in rural places like ... Alabama. Unsurprisingly, the Alabama medical board's proposed rule arose from a complaint by an anesthesiologist about a "disturbing situation occurring in several facilities in Alabama where … [a CRNA] was providing epidural steroid injections to patients." The anesthesiologist claimed this practice threatened patient safety and asked the Alabama Board of Nursing to stop it. The state nursing board ruled that the anesthesiologist appeared to have an economic interest in preventing nurses from performing these procedures, said the nurses were authorized to perform them and had been doing so for some time, and told the anesthesiologist to buzz off. The spurned doctor got a more sympathetic hearing from the more physician-centric State Board of Medical Examiners.
As the FTC letter notes, in proposing its pain rule, the Alabama medical board cited no evidence that letting nurses perform the tasks under discussion posed any dangers to patients. What evidence it could find pointed the other way. Earlier this year, the peer-reviewed journal Health Affairs ran an article under the self-explanatory headline "No Harm Found When Nurse Anesthetists Work Without Supervision By Physicians." The article drew on the experience of 14 states that let nurse anesthetists work unsupervised by doctors when treating Medicare patients. (The Medicare program has allowed this since 2001, provided the state's governor requests a waiver. According to the Health Affairs article, anesthesiologists successfully fought a version of this rule that didn't require the governor's involvement.)
The notion of allowing nurses and doctors' assistants to perform routine medical tasks in order to reduce medical costs and make certain services more widely available is controversial only to the particular doctors whose economic interests are at stake (and not even always to them). It has no discernable left-right valence, and the FTC has promoted it under presidential administrations both Democratic and Republican. In 2002, for instance, it sued the South Carolina Board of Dentistry when the dental board wouldn't allow hygienists into schools to clean and apply sealants to the teeth of low-income children (a group in whom dentists typically show little interest). The dental board signed a consent agreement five years later. George W. Bush, no regulatory zealot, was in the White House the whole time. When politicians get involved in such fights, the usual reason isn't ideology, but campaign contributions or electoral support from the affected doctors.
Under Obamacare, the need to curb medical inflation will be more urgent than it's been in the past, and almost none of the proposed solutions is as uncontroversial as letting nurses treat pain. But as the Alabama example demonstrates, some government agencies put interest-group needs ahead of consumers', and will throw up regulatory barriers to protect them.
Update, Nov. 12: This column has inspired more than the usual number of critical comments (see below), many from sensible-sounding people. Having reviewed these and then taken a second look at the above, I conclude that while I committed no errors that I know of, I let my readers down in three ways.
First, I should have made clear that while CRNAs are competent to do many things that anesthesiologists do, they are not necessarily competent to do everything that anesthesiologists do. (Even the Alabama nurse's board said CRNAs should not be permitted to make medical diagnoses, and admitted some doubt as to whether CRNAs could handle spinal facet joint injections.) I thought this point would be self-evident, but it wasn't.
Second, I should have clarified the distinction between "non-interventional" pain management such as administering pills, which goes unaddressed in the Alabama medical board's proposed rule, and "interventional" pain management, the somewhat more complicated procedures under discussion here.
Third, I shouldn't have compared the median salary for anesthesiologists ($211,750) with the median salary for registered nurses ($63,750). I should have compared the median salary for anesthesiologists with the median salary for CRNAs, a subset of registered nurses who have received specialized training. In my own defense, I was unable to find such a figure from the Bureau of Labor Statistics. But one commenter dug out an average salary figure of $189,000 from a 2009 survey by Merritt Hawkins & Associates, a health care consulting firm. Mindful that medians vs. averages constitute a poor basis for comparison, I nonetheless concede that if the average salary for CRNAs is $189,000 then the median CRNA salary is probably well into the six figures. The larger point remains. CRNAs make less money than anesthesiologists ($189,000 is less than $211,750), as you'd expect. So allowing CRNAs to perform more tasks performed by anesthesiologists would save money.
Update, Nov. 18: The Alabama State Board of Medical Examiners has "indefinitely postponed" the proposed rule, according to the Nov. 17 Birmingham News, pending completion of two national studies.
Thursday, December 16, 2010
CBC News - Health - Chronic pain affects 1 in 3 Canadians: poll
The SES Research survey found that 16 per cent of those surveyed report living in constant pain, and 20 per cent experience pain on a daily basis.
A family shovels snow. When study participants were asked to rate, between 0 and 10, the following statement: 'My family does not understand how pain affects my life,' 30 per cent scored between seven and 10.
(CBC)
The telephone poll of 2,000 Canadians was conducted for the Canadian Pain Society from Oct. 10 to 22. Respondents were asked whether they had chronic pain and how they rated the intensity of their pain.
Three hundred people who said they had moderate to severe chronic pain underwent additional in-depth interviews with SES interviewers.
"Pain is clearly having an enormous impact upon the lives of Canadians," said Nikita Nanos, president of SES Research, in a release. " A full third of individuals with moderate to severe pain said that they had lost their job as a result of it and half said that they had seen a reduction in income."
According to the poll, the income loss due to pain was estimated at $12,558 over a one-year time period.
Thirty-three per cent of Canadians surveyed said moderate or chronic pain makes them feel helpless.
It also revealed relationship and family issues associated with pain. When study participants were asked to give a score of between 0 and 10 to the following statement: "My family does not understand how pain affects my life," 30 per cent scored between seven and 10.
As for employment problems associated with chronic pain conditions, 33 per cent of respondents who suffer from moderate or severe chronic pain said they had lost their job as a result of their condition, while 25 per cent strongly agreed with the statement: "I fear my pain will cause me to lose my job."
http://www.cbc.ca/health/story/2007/11/07/chronicpain-study.html
Surgically implanted sensor uses iPhone technology to ease pain
Following a workplace accident more than four years ago, Donald Anderson was hit with excruciating pain that shot up his left leg.
He turned to surgery, chiropractic, physiotherapy and countless drug treatments; nothing helped. A 20-minute walk would leave him in agonizing pain.
But the 57-year-old Regina man says his pain has decreased by as much as 40 per cent -and his medication by 80 per cent -thanks to a wristwatch-sized device that uses motion-sensor technology similar to what's found in your iPhone or Nintendo Wii.
"Right off the bat, there was a noticeable improvement," Anderson says. "I sleep better, I can sit longer, walk farther -pretty much do everything with less pain than was the case previously."
Anderson and nine other Canadians with chronic pain have been implanted with the technology, developed by Minneapolis-based Medtronic and approved by Health Canada two months ago.
The device -called a RestoreSensor neurostimulator -sends out electric currents to automatically neutralize pain when it senses certain changes in the body's position.
Older models of neurostimulators require the patient to manually adjust the level of stimulation each time posture changes and pressure is shifted.
The motion-sensor technology -triggered in the same way an iPhone screen flips with a simple shift of the wrist -eliminates the need for frequent adjustment.
"It knows the position of the body ... all the time," says Dr. Krishna Kumar, a chronic pain expert and neurosurgeon with nearly 50 years experience who helped develop the technology.
The amount of fluid around each vertebrae of the spinal column changes as the patient sits, stands, walks or lies down, explains Kumar.
"The idea is that we stop the pain messages from getting to the conscious level so the pain will improve, the drug level will come down and the patient will get functionally better," says Kumar.
Kumar says about one per cent of the Canadian population -or 340,000 people -suffer from this kind of pain and could greatly benefit from the technology.
A Child in Pain: What Health Professionals Can Do to Help By Leora Kuttner
Now, finally, here is a book that will give you the practical strategies that are based on a sound comprehensive scientific framework. This volume is designed to help pediatric health professionals gain a true understanding of childhood pain. Pain is the most common reason for children to seek a medical consultation – and sometimes is the most common reason for avoiding it. Unaddressed fears and anxiety complicate pain management and recovery. This book comprehensively examines children's fears and anxieties that accompany their need for pain relief, and gives the professional the communication skills and words that can help calm these fears.
This book is addressed to all disciplines, and is organized into three parts: Part I explores the scientific understanding of pain as a part of children's development; Part II explores pain treatments themselves, their efficacies and how to combine them for therapeutic impact; and Part III uses this understanding to help translate knowledge into clinical practice in three major arenas of pediatric medicine: the physicians' office, the dentist's office, and in the hospital.
Wednesday, December 15, 2010
New miniature smart chip implant to combat chronic pain
The smart chip implant technology is officially called Implantable Neuro Sensing and Stimulation or INS2, and is designed to combat chronic pai. It has been developed over the last couple of years by National ICT Australia(NICTA) in Sydney. The development team of 10 includes biomedical experts, electrical and mechanical engineers, software developers, and experts in textile technology.
There are already devices that can be implanted to block pain, but according to NICTA's chief technology officer, Dr. John Parker, these are around the size of a matchbox, whereas the new implant is around the size of a single match head. Dr. Parker said the smaller size improves the reliability of the device and enables it to be implanted closer to the spine.
The new implant consists of one or two smart chips built into a biocompatible device about the size of the head of a match. The device is sewn into a 1.22 mm wide container of a polymer material with integrated electronic wires. The device is then implanted on the target nerve such as the spinal cord or elsewhere in the body. The device is operated by an internal computer processor run by a battery the size of a SIM card that can be recharged wirelessly. Wireless recharging means there is no need for external wires or devices.
The device monitors the properties of the nerves carrying pain signals to the brain and can be "fine-tuned" to block the undesirable pain signals with electrical pulses of up to 10 volts. Since the pain signals no longer reach thebrain, there is little or no sensation of pain. The device will be able to manage different levels of pain in different ways.
NICTA said the device may have numerous applications apart from treating chronic back pain or leg pain, and could be used to block pain caused by nerve damage and migraines. It also has the potential to help control epileptic seizures and the tremors caused by Parkinson's disease.
http://www.physorg.com/news/2010-12-miniature-smart-chip-implant-combat.html
Friday, December 10, 2010
Maybe It's Fibro? Webinar Series - American Pain Foundation
Tuesday, December 07, 2010
Fish Feel Pain Too : Discovery News
In her book "Do Fish Feel Pain?" (Oxford University Press, 2010), Braithewaite presents her case that fish, like most other organisms, are capable of experiencing pain and that humans can cause fish to suffer.
Here at Discovery News we've covered similar research that concluded lobsters, crab and other shellfish feel pain too. For me, it would be a surprise if they didn't, but scientists have been struggling for ways of proving the obvious here. I think Braithewaite does a good job of summarizing the latest findings.
Braithewaite found that fish have the same kinds of specialized nerve fibers that mammals and birds use to detect noxious stimuli, tissue damage and pain. She also explored whether fish are sentient beings and whether an organism must possess "awareness" to experience pain.
"We now know that fish actually are cognitively more competent than we thought before -- some species of fish have very sophisticated forms of cognition," she said in a press release. "In our experiments we showed that if we hurt fish, they react, and then if we give them pain relief, they change their behavior, strongly indicating that they feel pain."
She was initially drawn to the issue after reading about fish-farming concerns.
"By 2030, half of all fish that humans eat will come from fish farms," she said. "It seemed logical to me to care about fish, because agriculture in general is confronting animal-welfare issues. If we are concerned about animal welfare, we should be concerned about fish welfare."
She believes the United States is 10 years behind Europe now in its thinking about the way it keeps and kills animals in agriculture. Those concerns are just now starting to be extended to aquaculture.
"Electrical stunning may change the way we harvest fish at sea," she said. "We have a responsibility, I think, to make clean and quick kills of fish we eat. Certainly, most of us are not comfortable with piles of fish slowly suffocating on the decks of fishing trawlers at sea and in port. People are rightly asking: 'Isn't there a better way?'"
To do this on a widescale, commercial level, protections related to pain and suffering that are now given to birds and mammals should be widened to include fish.
"There is a perception that fish have simple brains and are incapable of feelings, and this has somehow made them different from birds and mammals when it comes to our concerns for their welfare," she said. "But we now have strong evidence that suggests fish are more intelligent than previously thought and their behavior more complex."
Saturday, December 04, 2010
Novel approach to chronic pain relief
Previously, scientists have been able to show that a protein molecule known as PKM zeta is required to store memories. In the case of chronic pain, there is a malfunctioning in the neural process that stores those memories, which prevents the brain from adapting the subsequent behavioural response which would ordinarily allow it to cope with the pain. The connections between neurons through synaptic pathways in the central nervous system are somehow flawed, causing an individual to re-experience pain as the mental record of that pain persists.
This new research has detected the cause for this malfunction and in doing so, has identified a novel target for the treatment of neuropathic pain. By inhibiting PKM zeta in a part of the brain involved in the perception of pain in a mouse model, the international team of scientists have been able to eliminate the painful memory responsible for chronic pain.
Professor Graham Collingridge, from the University of Bristol's MRC Centre for Synaptic Plasticity, the School of Physiology and Pharmacology, and part of the Bristol Neuroscience network, said: "If this translates to humans, it may be possible one day to treat some forms of chronic pain by inhibiting PKM zeta or other molecules involved in the storage of the painful memory. The challenge will be to target the drug so that it inhibits painful memories but not other forms of memory. "
By studying how brain connections operate in a part of the cortex involved in pain sensation in mice, the team found that the molecule PKM zeta actually serves to maintain pain-induced persistent changes in the brain, thereby prolonging the sensation of chronic pain.
The team combined biochemistry, electrophysiology and behaviour to study the role of PKM zeta in the anterior cingulate cortex, a brain region known to be activated in humans during painful states. The identification of a molecular basis for chronic pain provides a framework for the development of more effective therapies in the future.
http://www.sciguru.com/newsitem/5155/Novel-approach-to-chronic-pain-relief/
Tuesday, November 16, 2010
Fruit flies lead scientists to new human pain gene
Understanding the genetic basis of pain will lead to the development of new analgesics, the identification of risk factors for chronic pain and improved decision-making about the suitability of surgical treatment for different patients, says Clifford Woolf, MB, BCh, PhD, the study's senior co-author and director of the F.M. Kirby Center and Program in Neurobiology at Children's.
Classic studies of twins indicate that about 50 percent of variance in pain sensitivity is inherited. "Across a number of different kinds of pain, genes seem to be at least half the driver of how much pain you experience," Woolf says. "Genes give us an amazing and powerful tool to begin to understand how pain is generated, and which functional pathways and specific proteins are involved."
The new gene, discovered in a collaboration with the Institute of Molecular Biotechnology of the Austrian Academy of Sciences and others, encodes part of a calcium channel called alpha 2 delta 3 (α2δ3). Calcium channels are pores in the cell membrane through which calcium ions pass, and are critical for the electrical excitability of nerve cells.
The study, co-led by Joseph Penninger, PhD, scientific director of the Institute of Molecular Biotechnology in Vienna, took advantage of the relative ease of conducting genetic screens in fruit flies. Nearly 12,000 genes were targeted for mutations specifically in nerve cells, using RNA interference (RNAi) technology. The team then exposed the different mutant flies to noxious heat, and identified the ones that failed to fly away. After eliminating flies with other complications, such as an inability to see or fly, they zeroed in on those with mutations that appeared to be specific to pain.
Of the nearly 600 candidate pain genes identified, α2δ3 was one chosen for further study, in part because calcium channels are a known target of some existing analgesics. (Another member of the α2δ family of calcium channels, α2δ1, is a target of gabapentin and pregablin, commonly prescribed for neuropathic pain.)
Studies of mice lacking α2δ3 demonstrated that this gene controls sensitivity to noxious heat in mammals as well as flies. Further, functional MRI imaging of the mutant mice revealed that α2δ3 controls the processing of thermal pain signals in the brain: the heat pain signal seems to arrive appropriately at the thalamus, an early processing center, but does not travel to higher order pain centers in the cortex. Instead, the MRI images showed a surprising cross-activation of vision, olfaction and hearing cortical areas. This cross-activation, or synesthesia, was noted with tactile stimulation in addition to the heat pain stimulus.
More ...
http://www.labspaces.net/107635/Fruit_flies_lead_scientists_to_new_human_pain_gene
How Pain Can Make You Feel Better: Scientific American
This is called nonsuicidal self-injury (NSSI), and it most commonly takes the form of cutting or burning the skin. Traditionally, many doctors, therapists, and family members have believed that people engage in NSSI primarily to manipulate others. However, recent research has found that such social factors only motivate a minority of cases and usually represent cries for help rather than coldhearted attempts to exploit caretakers. Although there are many reasons why people engage in this kind of self-injury, the most commonly reported reason is simple, if seemingly odd: to feel better. Several studies support the claim that self-inflicted pain can lead to feeling better. For example, Schmahl and colleagues scanned the brains of people with a history of NSSI during a painful experimental task designed to mimic NSSI. They found that the pain led to decreased activity in the areas of the brain associated with negative emotion. The reality of this effect provokes a perplexing question: How could self-inflicted pain possibly lead to feeling better?
One possible answer to this question is that some people are simply hard-wired to like pain. Although NSSI is associated with an increased pain threshold and tolerance, people who engage in NSSI still report feeling pain and, furthermore, report that this pain is unpleasant. Moreover, if these people are hard-wired to like pain, it is unclear why they primarily engage in NSSI when stressed or why they stick to moderate self-injury (e.g., cutting the skin) rather than severe self-injury (e.g., limb amputation).
Another possible answer is that these people want to punish themselves and that they simply like punishment. It is true that self-punishment is a commonly reported reason for engaging in NSSI; however, by definition, punishments increase negative emotion and make a behavior less likely to occur in the future. Thus, self-punishment may motivate some of these people, but self-punishment cannot be the reason that NSSI reduces bad feelings. During NSSI, something else must accompany the negative emotion associated with self-punishment and pain. Exciting new research now suggests that this "something else" is the relief that occurs when something that causes acute, intense pain is removed.
To illustrate this effect, imagine that one morning you visit the doctor for a routine check-up, and later that afternoon the doctor's office calls to inform you that you're in the advanced stages of cancer and have weeks to live.... Now imagine that the doctor's office calls back five minutes later and tells you that they mixed up your lab work with someone else's – you're actually in good health. You would not immediately go back to how you felt before the first phone call; rather, you would feel extreme relief, lasting for hours or even days. Note that it was not a reward (e.g., winning the lottery) that made you feel better, only the introduction and removal of something unpleasant.
New research suggests that the introduction and removal of physical pain may have a similar effect. Tanimoto and colleagues found that fruitflies avoided odors associated with the introduction of a shock, but approached odors associated with the removal of a shock. Similarly, Bresin and colleagues found that the removal various forms of experimental pain were associated with a reduction in negative emotion in people with no history of NSSI. This relief effect was particularly strong for people who had higher levels of negative emotion. This latter finding may help to explain why people with higher levels of negative emotion are more likely to engage in NSSI: they have more negative emotion to reduce, and thus more relief to gain. Using biological measures, Franklin and colleaguesobtained similar effects in both people with and without a history of NSSI. These new findings are especially interesting because it turns out that both general negative emotion and pain-induced negative emotion are processed in the same brain areas. This means that pain relief and emotional relief are essentially the same thing. Indeed, it was recently shown that pain relievers like acetaminophen also relieve emotional pain.
Many people find that it's hard to get emotional relief with traditional strategies (e.g., talking with friends). Consequently, they may resort to generating pain relief in order to generate emotional relief. Unfortunately, this also means that they have to generate acute, intense pain; that is, they have to engage in NSSI. Despite being an effective emotion relief strategy, NSSI is also a health-risk behavior that is associated with an increased risk of suicide. In short, NSSI can be a good thing for temporary emotional relief, but it's a bad thing for health.
The vast majority of people who engage in NSSI are not seeking to manipulate anyone and they're not wired differently than the rest of us. They simply tap into the natural emotional relief that accompanies the removal of intense, acute pain. They do this because they have trouble finding healthier ways to reduce their stress. Accordingly, ostracizing people who engage in NSSI only creates more stress and makes NSSI worse. The best way to help someone who engages in NSSI is to guide them to healthier ways to feel better.
http://www.scientificamerican.com/article.cfm?id=how-pain-can-make-you-fee&print=true
Wednesday, November 10, 2010
The Body Chronic
Being a little older and a lot wiser, I decided that no person should go through what I went through to get the basic information and support necessary to navigate the waters surrounding chronic illness. I started this blog in the hopes of creating a support network for those who have a daily interaction with The Body Chronic.
Tuesday, November 09, 2010
International Association for the Study of Pain | Low-Resource Guide
Topics range from the physiology and psychology of pain and principles of palliative care to management of patients with specific pain problems including various types of cancer, AIDS, sickle cell anemia, neuropathic pain, back pain, and visceral pain. Case reports provide illustrations of typical cases in the low-resource (often rural) setting in developing countries.
World-renowned experts provide chapters on setting up a pain management program, accessing resources for ensuring opioid availability, and setting up guidelines for local requirements. Authors with extensive clinical experience consider the integration of traditional medicines, modern pharmacotherapy (with consideration of the most cost-effective and readily available options), and techniques such as nerve blocks and radiation therapy.
http://www.iasp-pain.org/AM/Template.cfm?Section=Home&TEMPLATE=/CM/HTMLDisplay.cfm&CONTENTID=11669
Sunday, November 07, 2010
The Headache That Wouldn’t Go Away - NYTimes.com
In the emergency room, the young woman was sleepy and confused. She didn't remember the seizure. All she knew was that she felt bad earlier that day. Her shoulders ached and she had these strange shooting pains that ran up her neck, into her skull. She had a wicked headache too. Although she had this headache for months, it was much worse that day. At home she took a long hot bath and went to bed. She woke up in the ambulance.
She'd had no fever, she told the E.R. doctor, and hadn't felt sick — just sore. And now she felt fine. Her arm didn't hurt — in fact she couldn't remember that it had ever hurt. She still had the headache, though. She didn't smoke, didn't drink and took no medications. She moved to Boston from Bolivia several years earlier to get married and now had 15-month-old. Other than mild confusion, the patient's physical exam was normal. The E.R. doctor ordered blood tests to look for evidence of infection along with a CT scan of her head to look for a tumor.
Her headache started the year before, when she was pregnant. Before that she had the occasional headache, but back when her daughter was barely a bump, she got one that simply never went away. She told the midwife, who said it wasn't unusual to get headaches during pregnancy. But to the patient, this headache seemed different. It was like a vise on her head, just over her eyes. The pressure wasn't excruciating, just unrelenting. She took Tylenol, and that sometimes helped, but the headache always came back. Sometimes it even woke her up in the middle of the night. Finally the midwife sent her to her primary-care doctor.
Her doctor, a young internist in her first year of training (who asked that her name not be used), was worried about this headache. It had persisted for weeks and woke her patient up from sleep — that was unusual. The doctor recalled how happy the patient was when she called her with the news of her positive pregnancy test. And now barely showing at five months, she looked like the picture of expectant health. Had she had any weakness or numbness? Was there any loss of hearing or blurry vision? No, no and no. Well, she did have blurry vision, but that's only because she hated wearing her glasses.
The doctor focused her exam to look for any hint that this headache might be because of some kind of brain injury. She looked into the patient's eyes with the ophthalmoscope, scanning the retina for any signs of increased pressure inside the brain. She checked the patient's strength, coordination and reflexes. Nothing. Her exam was completely normal.
Headaches are common, accounting for some 18 million doctor visits a year. Most are completely benign, but up to 3 percent of patients with a headache severe enough to send them to the emergency room will have something worth worrying about. Doctors are taught to look for three types of potentially dangerous headaches: the first, the worst and the cursed. The first headache in someone who doesn't have headaches; the worst headache ever in someone who does; or a headache "cursed" by symptoms like weakness or numbness. A CT scan should be considered for these possibly life-threatening headaches. This headache fit into none of these informal categories.
This patient was woken up from sleep by her headaches — that's unusual, but the doctor knew that it was not one of the recommended reasons for getting a CT scan. And she was pregnant. A CT scan of the head requires a relatively high dose of radiation. Was the doctor's concern great enough to risk exposing the fetus based only on this somewhat unusual symptom? Not yet. Especially since there was another possible cause of the persistent headache — eyestrain. The patient was no longer wearing her glasses; she didn't even own a pair, she confessed. She should get new glasses, the doctor suggested, and see if wearing them helped her headache. If not, she should come back. Perhaps they would get a CT scan at that point.
It was more than a year later when the patient next came to see the doctor. She had gotten glasses, and though the headaches hadn't stopped, they seemed a bit better. It was no longer a constant pain. She had one maybe three to four times a week, and it lasted for a few hours and went away with a little ibuprofen. Besides, she was really too busy with the baby and her job to worry too much about them.
Then, six months after that last visit, she had this middle of the night seizure. In the E.R., the blood tests were all normal. Not so the CT scan. On the right side of the patient's brain, just over the eye, there was a bright circle of white, the size of a dime. Not a brain tumor. No, the radiologist said, this was a tiny worm, a larvae, the young offspring of a tapeworm. The parasite, known asTaenia solium, is transmitted through undercooked pork contaminated by tapeworm eggs. Once in the body, the eggs hatch and then attach themselves to the intestinal wall and within a few months can grow to up to 15 feet or more. A mature tapeworm will then release hundreds of eggs into the gut every day. If any of these are ingested, they can hatch, enter the bloodstream and, once there, can lodge almost anywhere in the body, although they usually end up in muscle and in the brain.
Although unusual in the United States, pork tapeworm is common in the developing world. And having these larvae in the brain, a condition known as neurocysticercosis, is the most common cause of adult epilepsy in South and Central America. The patient was probably infected with this tapeworm years earlier when she lived in Bolivia. This kind of infection can be asymptomatic for years. Once the doctors saw the CT scan, the patient was treated with an antiparasite medication for 30 days and started on antiseizure medications.
When her primary-care doctor heard that her patient had been diagnosed with neurocysticercosis, she scoured the patient's hospital chart and then her own notes. How had she missed that? What should she have done differently? She discussed the case with several of her teachers, who assured her that she had done everything properly. One of the frustrating truths in medicine is that it is possible to do everything right and still be wrong and miss the diagnosis.
The young doctor called the patient to see how she was doing and to schedule a follow-up visit. She was disappointed, though not completely surprised, when the patient chose to see a different doctor at the clinic.
In thinking about this case, the doctor's greatest regret is that she didn't get the chance to follow up on her patient and find out that her headaches didn't go away by just wearing glasses. When patients don't come back, the temptation is to assume they've gotten better. That is often not the case. Sometimes they've just given up. Now when she has a patient she is worried about, the doctor doesn't tell them to call her if they don't get better. Instead she has them make an appointment to come back in a couple of weeks. "If they are all better," the doctor told me, "they can cancel the appointment. But just in case they aren't — the way this woman wasn't — they can come back, and I can have another shot at the whole thing."
Lisa Sanders is the author of "Every Patient Tells a Story: Medical Mysteries and the Art of Diagnosis."
http://www.nytimes.com/2010/11/07/magazine/07FOB-Diagnosist-t.html?ref=magazine
Monday, November 01, 2010
StumbleUpon - Discover - Pain
Sunday, October 31, 2010
Pain: MedlinePlus
You can use MedlinePlus to learn about the latest treatments, look up information on a drug or supplement, find out the meanings of words, or view medical videos or illustrations. You can also get links to the latest medical research on your topic or find out about clinical trials on a disease or condition.
Thursday, October 28, 2010
Global Year Against Acute Pain - International Association for the Study of Pain
- Disseminate information about acute pain worldwide
- Educate pain researchers as well as health care professionals who see the issues associated with acute pain first-hand in their interactions with patients
- Increase awareness of acute pain among government officials, members of the media, and the general public worldwide
- Encourage government leaders, research institutions, and others to support policies that result in improved pain treatment for people with acute pain
Tuesday, October 26, 2010
In pain? Don't let your GP fob you off with pill... | Mail Online
Twenty years after Ian Semmons was badly injured trying to prevent a robbery, he is still in pain. Thrown down a flight of stairs, he'd shattered his back and ankles.
Despite two-and-a-half years of operations and rehabilitation — and strong painkillers — he lived in constant agony from his shoulders to his ankles.
'At its worst, it was like having big, sharp needles thrust into your body,' recalls the former risk management consultant.
Ian is one of nearly 10 million Britons who suffer from chronic pain, which is defined as continuous, long-term pain of more than 12 weeks.
Worryingly, a new survey has found that people in the UK wait, on average, three years for a diagnosis of what's causing their pain, and a further three years before the pain is adequately managed.
In many cases, chronic pain affects sufferers' ability to work: four in 10 are unable to work at all, according to the Pain Proposal European Consensus Report funded by Pfizer. Pain is a natural response to injury.
Rather like sending a telegram, the damaged nerves transmit tiny messengers called neurotransmitters to the spinal cord — the body's superhighway — and then to the brain, which decides how to respond.
As the injury heals, the messages become less intense and less frequent, and finally stop. But this mechanism can go awry. Like a broken record, it keeps repeating itself, re-sending the messages of pain long after the reason for stimuli has passed.
A quarter of people affected by chronic pain suffer from depression, and many feel their pain is so bad that at times they want to die.
Yet sufferers are very much neglected in the UK, because GPs are uninformed about chronic pain and designated pain clinics, says Dr Beverley Collett, a consultant in pain medicine at the University Hospitals of Leicester and chair of the Chronic Pain Policy Coalition.
'Many healthcare professionals don't know enough about chronic pain,' she says.
'During their five to six years of medical school, doctors spend just 13 hours on pain. Nurses spend just 10 hours, and physiotherapists manage to clock up 35 hours.
'But this is simply not enough time to understand this complex problem.'
Yet there is more reason than ever for young medics to take this part of their training seriously, she says, as experts are at last discovering that chronic pain is not just the body failing to heal, or, worse, a psychosomatic 'cry for help'.
'For a long time, patients who complained of chronic pain were labelled with depression,' says Dr Collett. 'Now, we are realising they may be suffering what we call a hyper-excitable response within their bodies.
'This means that nerves in the area of original damage have become so sensitive to stimulus they keep reporting sensations back to the brain — even when nothing is going on to warrant a message. In turn, the brain interprets that message as pain.'
Once activated, this has a knock- on effect, causing other nerves to fire off pain messages, too.
In many cases, chronic pain affects sufferers' ability to work: four in 10 are unable to work at all
How well chronic pain is managed depends very much on how well your GP understands the condition — and whether you live close to one of the UK's few chronic pain clinics.
Like many patients, it was three years after the initial incident before anyone recognised that Ian's acute condition had become a long-term pain problem. He'd been effectively left to manage, with his GP prescribing the strongest painkillers month after month.
By the time he was referred to a pain clinic, after changing GPs, the active fortysomething man had become angry and frustrated — unable to work or even to play with his then five-year-old daughter Becky.
His marriage had broken down, as his wife was unable to cope with the change to her husband.
'It was only when I got to see a consultant in pain medicine that anyone explained to me that I was going to be in pain for the rest of my life. Ironically, this was more of a mental boost than it sounds, as he told me I had to accept that I was not going to "recover" in the accepted sense, and that I had to get on with my life again.'
But the real improvement came 14 months later, when Ian was referred to a psychiatrist. 'I had reached rock bottom by the time I saw him. I had even taken to hiding a pack of very strong painkillers so that I could end my life if it all got too much.
'But the counselling helped me to move forward and finally to reduce the amount of medication I took, which itself was making me moody and physically uncomfortable.'
Side-effects of strong painkillers include constipation, insomnia and nausea — and Ian had suffered the whole range.
'With counselling, I started to focus on what I could do, not what I couldn't. My daughter motivated me, too. I didn't want her to miss out on having a dad.'
A crucial part of his recovery probably can't be replicated by most patients: he married his former physio, 47-year-old Judith, and the couple now have a 12-year-old son, Thomas.
But Ian, now 60, admits that 20 years on from the original incident, he is still in pain every day — and knows he always will be.
'I still need regular operations to relieve scar tissue, and I have rotten arthritis, too. But I mostly only use a stick these days, not crutches, and rarely take more than paracetamol.'
Ian went on to found the country's largest general pain charity, Action On Pain, and now campaigns for better service. 'Over 90 per cent of callers to our helpline don't even know pain clinics exist,' he says.
Dr Collett says it's essential patients see a pain specialist in conjunction with other experts.
'In Leicester, we are well equipped with a wide multi-disciplinary team, from anaesthetists to physiotherapists, as well as specialist pain nurses and consultants, but that is just not true everywhere.'